Pandemic Disproportionately Drove Dually Eligible Medicare-Medicaid Beneficiaries to Skilled Nursing Facilities: Lessons from COVID-19

The nearly 15,000 skilled nursing facilities (SNFs) across the United States played a critical role in the nation’s early response to the COVID-19 public health emergency. However, given high COVID-19 infection rates in SNFs, there was a strong preference to discharge hospitalized patients home rather than to SNFs during the first year of the pandemic.
Using claims data before and during the pandemic (2017–21), this analysis examined SNF admissions among Medicare fee-for-service beneficiaries who were dually eligible for Medicare and Medicaid and beneficiaries who were eligible only for Medicare. Dually eligible beneficiaries—compared to Medicare-only beneficiaries—tend to have lower incomes and fewer assets, are more likely to qualify for Medicare due to a disability, and are much more likely to be in fair or poor health.
Following the start of COVID, Medicare-only beneficiary SNF admissions dropped markedly, while SNF admissions for dually eligible beneficiaries increased. In sum, the most vulnerable Medicare beneficiaries—those dually eligible for Medicaid—were much more likely to be discharged to high-risk SNF settings early in the pandemic than Medicare-only beneficiaries.
Both dually eligible and Medicare-only beneficiaries are covered for medically necessary Medicare home health services, including part-time skilled nursing; physical, speech, and occupational therapy; and part-time home health aide services. Therefore, other factors like illness severity, lack of caregiver support at home, or greater health-related social needs may have contributed to greater SNF use by dually eligible beneficiaries. Understanding why dually enrolled Medicare beneficiaries were disproportionately discharged to SNFs can help policymakers improve care for this vulnerable population because they account for a large and disproportionate share of health care spending.
From the Data Point: Number and Percentage of Skilled Nursing Facility (SNF) Admissions, by Medicare-Medicaid Dual Eligibility Status, Q1 2017–Q4 2021
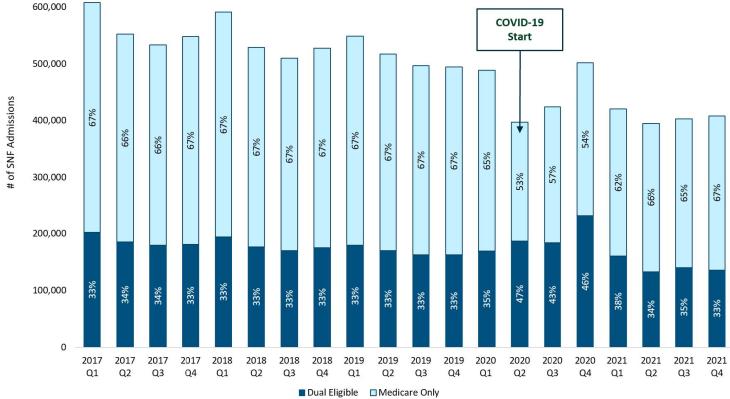
Key Findings
- At the start of the COVID public health emergency—from first to second quarter 2020—SNF admissions dropped 34 percent for fee-for-service beneficiaries with only Medicare coverage, while SNF admissions increased 10 percent for beneficiaries covered by both Medicare and Medicaid.
- Dually eligible beneficiaries—who make up less than 20 percent of all FFS Medicare beneficiaries—accounted for nearly half of all SNF admissions during the 2020 pandemic peak before returning to a one-third share of SNF admissions in 2021—the same as before the PHE.
- The results indicate that dually eligible beneficiaries were more severely affected by the COVID public health emergency and had a more challenging recovery than Medicare-only beneficiaries.


